Multiple Sclerosis – What are the symptoms and treatment?
Author: Lucie Garabasova
Multiple sclerosis (MS) is an autoimmune disease of the brain and spinal cord (central nervous system) that can cause disability. In MS, the immune system attacks the protective sheath (myelin) that covers nerve fibers, causing communication problems between the brain and the rest of the body.
Multiple sclerosis is divided into four groups (based on symptoms). The classification determines the appropriate treatment. CBD hemp is also suitable for alleviating symptoms. We will introduce you to how it can help.
What is Multiple Sclerosis?
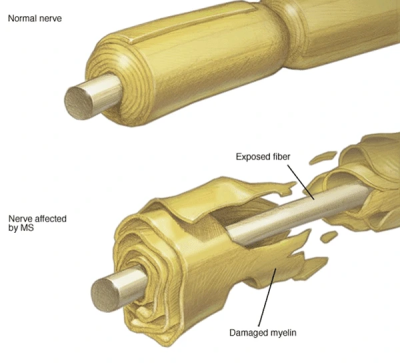
As mentioned above, multiple sclerosis – abbreviated as MS – is an autoimmune disease. The image below clearly shows what this disease causes:
The body's own immune system attacks the protective sheath covering nerve fibers. A damaged sheath causes communication problems between the brain and the rest of the body. MS symptoms and signs vary widely depending on the extent of nerve damage and which nerves are affected. Some people with severe MS may lose the ability to walk independently, while others may experience long periods of remission (symptom-free phases) without new symptoms.
Multiple sclerosis cannot be completely cured. The primary goal of treatment is to alleviate symptoms, prevent new attacks, slow disease progression, and prevent disability.
Types of Multiple Sclerosis
In 1996, the American National Multiple Sclerosis Society standardized the definitions of four forms of MS.
- Relapsing-Remitting (RR) MS – The most common form of MS (85–90% of patients). It is characterized by alternating attacks and remissions and typically lasts several years. Symptoms usually persist for a short time and then partially or completely subside.
- Secondary Progressive MS – Symptoms worsen over time as the body exhausts its regenerative capacity. The transition from the first to the second form of MS typically occurs within 19 years.
- Primary Progressive MS – Affects about 10–15% of patients who have never experienced a remission after the initial symptoms. It is characterized by a slow progression of symptoms and disability from the onset, with minimal or no improvement. It usually develops in patients around the age of 40–50.
- Progressive-Relapsing MS – The rarest and least common form of MS. It is progressive from the start, and after relapses, there is little to no improvement, with each attack causing permanent neurological damage. It is the most difficult form to treat and typically leads to disability within a few years, most commonly affecting people over 40 years old.
Orange is the official color of MS awareness. World Multiple Sclerosis Day is observed annually on the last Wednesday of May.
Experts estimate that about 20,000 people in the Czech Republic have multiple sclerosis.
What are the symptoms of Multiple Sclerosis?
Symptoms and signs of multiple sclerosis can vary widely among individuals and over the course of the disease, depending on which nerve fibers are affected.
Common symptoms affecting movement include:
- Numbness or weakness in one or more limbs, usually occurring on one side of the body or in the legs and torso
- Electric shock sensations occurring with certain neck movements, especially when bending the neck forward (Lhermitte’s sign)
- Tremors, lack of coordination, or unsteady walking
Vision problems are also common, including:
- Partial or complete loss of vision, usually in one eye, often with pain during eye movement
- Prolonged double vision
- Blurred vision
Other symptoms of multiple sclerosis may include:
- Slurred speech
- Fatigue
- Dizziness
- Tingling or pain in various parts of the body
- Problems with sexual function, bowel function, and bladder control
Treatment of Multiple Sclerosis
Currently, multiple sclerosis cannot be cured, but various treatment approaches help control its progression and alleviate symptoms.
Treatment depends on the specific symptoms and difficulties experienced by the patient. Generally, it includes:
- Short courses of steroid medications to speed up recovery
- Specific treatments for individual MS symptoms
- Disease-modifying therapies to reduce the frequency of relapses
When to see a doctor?
If you experience any of the above symptoms for unknown reasons, do not wait and visit a doctor.
Multiple Sclerosis Diagnosis
There is no single reliable test to diagnose MS. Instead, doctors use multiple criteria based on various examinations. These diagnostic criteria are outlined in a document called "McDonald Criteria," named after the doctor who led a panel of experts in 2001 to establish precise diagnostic criteria for MS. These criteria are regularly updated as research progresses and understanding of the disease improves, aiming for more accurate and faster diagnoses while reducing the risk of misdiagnosis.
As part of the diagnostic process, a healthcare professional gathers the patient’s medical history and supplements it with imaging and laboratory tests. To confirm an MS diagnosis, the doctor must:
- Identify the number of "attacks" of the disease (dissemination in time and space)
- Confirm damage to the central nervous system in at least two different areas (dissemination in space)
- Confirm that the damage occurred at two different times with at least a one-month gap (dissemination in time)
- Rule out other diseases that could cause similar symptoms
Multiple Sclerosis and Blood Tests
Although there is no definitive blood test for MS, blood tests can rule out other conditions with similar symptoms, such as Lyme disease, other autoimmune diseases (vasculitis), certain rare hereditary disorders, and AIDS.
Disease progression
Most people with MS have a relapsing-remitting course of the disease. They experience periods of new symptoms or relapses lasting for days or weeks, which usually improve partially or completely. These relapses are followed by quiet remission periods, which can last months or even years.
Worsening symptoms usually involve mobility and walking difficulties.
What causes Multiple Sclerosis?
The cause of multiple sclerosis is unknown.
It is unclear why some people develop MS while others do not. The most likely explanation is a combination of genetic and environmental factors.
Risk Factors That May Increase the Risk of Developing Multiple Sclerosis
- Age – MS can occur at any age, but its onset typically occurs between 20 and 40 years old. However, younger and older individuals can also be affected.
- Gender – Women are two to three times more likely to develop relapsing-remitting MS than men.
- Family History – If a parent or sibling has MS, there is a higher risk of developing the disease.
- Certain Infections – Several viruses, including the Epstein-Barr virus (which causes infectious mononucleosis), are associated with MS.
- Vitamin D Deficiency – Low vitamin D levels and limited sun exposure are linked to a higher risk of MS.
- Autoimmune Diseases – Individuals with autoimmune diseases such as thyroid disease, pernicious anemia, psoriasis, type 1 diabetes, or inflammatory bowel disease have a slightly higher risk of MS.
How can CBD help people with Multiple Sclerosis?
Multiple sclerosis is an autoimmune disease, and CBD works within the immune system.
CBD can help alleviate several MS symptoms, including:
- Fatigue
- Mobility
- Pain
A 2018 scientific study found that CBD reduces pain, fatigue, inflammation, and depression in people with MS while also improving mobility. The authors concluded that CBD supplementation would be beneficial for MS patients.
Does CBD have side Effects for MS Patients?
Like any other supplement or medication, CBD may have side effects in some individuals, such as:
- Drowsiness
- Dizziness
- Low blood pressure
Additionally, CBD may interact with other prescription medications. Consult your doctor before using CBD. Most MS specialists are familiar with CBD, as at least 20% of MS patients currently use it.
How to use CBD for Multiple Sclerosis?
CBD can be taken in the form of CBD oils, capsules, or vaporization of flowers – it all comes down to your personal preference and what suits you best.
When it comes to dosage, start gradually. Always take it for several days, and if you feel that you haven’t achieved the desired effect, increase the dosage and continue this process.
According to available studies, taking 300 mg of CBD daily for six months is considered safe. To give you an idea, this means you can take up to 35 drops of 20% CBD oil daily and still stay within the 300 mg daily limit. Most patients do not require such a high dosage—typically, patients with MS use around 60 mg of CBD daily (13 drops of 10% CBD oil).
As mentioned above, in addition to CBD, incorporating CBG oil is also recommended to enhance the overall effect.
Life with Multiple Sclerosis and Medical Cannabis
To conclude, here is the story of a man who has been living with multiple sclerosis for 24 years and has significantly benefited from medical cannabis.
"I am a person diagnosed with multiple sclerosis. Over the years, many people have asked me what life with MS is like and what treatment I use (personally, medical cannabis has helped me a lot). I will try to give you an insight into life with MS.
In 1998, I was diagnosed in the early stages with secondary progressive MS. My symptoms included flu-like signs leading to loss of control over certain parts of my body. At one point, it was my urinary tract, forcing me to use the toilet at every possible opportunity. My legs were losing strength, and my eyes were also affected—one episode even caused blindness in one eye and significant vision loss in the other.
I was not a Czech citizen during the first two years of my treatment, which made access to healthcare (financially) difficult. However, in 2000, that changed, and I was finally included in the health insurance system, allowing my treatment to proceed properly. I received all available diagnostics and treatments, including steroid therapy with Prednisone, Medrol, and Azathioprine (a very strong immunosuppressant used in organ transplants to prevent rejection). This was part of a study on the use of this drug in MS treatment. Its effectiveness was monitored using MRI (magnetic resonance imaging), which led to another long-term project monitoring MS progression (providing over 10 years of valuable medical data).
I received various cytostatic chemotherapeutic agents in the form of infusions (presumably to eliminate microorganisms triggering my immune response), as well as beta interferon A drugs—Avonex (for 9 months) and Rebif (for 2 years), which involved regular biweekly injections.
The result of these treatments was that my body suffered like never before. I felt as if my cells were breaking down, my senses "felt" the attacks of my immune system, I experienced chronic fatigue syndrome, and an almost insurmountable overall weakness.
When my son was born, my life gained new meaning, and he became my reason to fight even harder against this disease. It occurred to me to try cannabis in addition to conventional treatment—medical cannabis, which I grew myself. I started using it, and between 2006 and 2007, my classification changed from chronic progressive MS to relapsing-remitting MS, which, according to my neurologist, does not happen often and was likely due to cannabis.
Now, seven years later, I am a fully functional working member of society, though still marked by a noticeable limp and walking with a cane. It feels as if I’ve been through a war—which, in a way, I have. A war with myself."
Source of the patient’s story on medical cannabis: Legalizace Magazine.